What is Ectopic Pregnancy?: Symptoms, Causes & Treatment
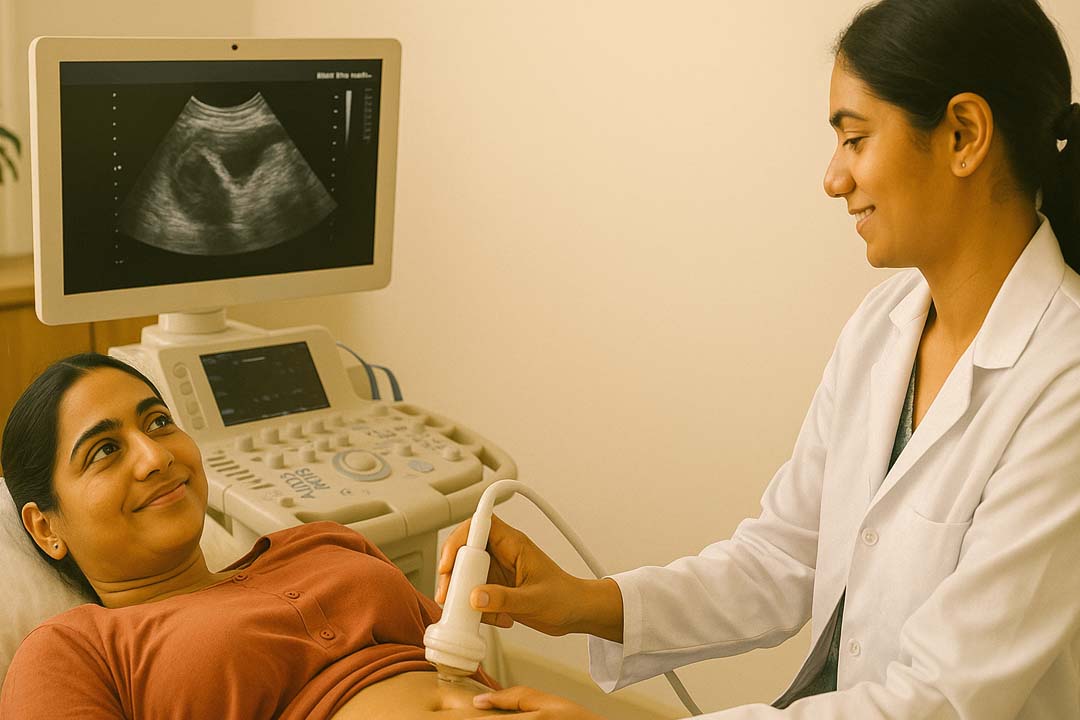
Fertility evaluations don’t always start with complex treatments. Often, the first task is to check whether the “pathway” from the ovary to the uterus is open and healthy. Sonosalpingography which is commonly called SSG does exactly that.
It’s an ultrasound-based scan where a small amount of sterile fluid (sometimes a specially designed ultrasound contrast foam) is gently infused into the uterus while the clinician watches in real time.
If the fluid flows through and “spills” from the ends of the fallopian tubes, the tubes are considered open and if not, a blockage may be present. Because it uses ultrasound rather than X-rays, SSG avoids radiation and allows the uterus and ovaries to be reviewed during the same sitting.
The scan is brief, usually performed as an outpatient visit, and most people return to routine activities straight after. In short, SSG offers a quick, radiation-free look at the tubal pathway to guide next steps in a fertility work-up.
Why is SSG Important?
SSG shows whether fluid can pass through the fallopian tubes, and at the same time provides a close ultrasound look at the uterus and ovaries which are key information early in a fertility evaluation.
When tubes are open (“patent”), eggs and sperm can meet; when one or both tubes are blocked, natural conception may be less likely and treatment plans change.
SSG (also called HyCoSy when contrast is used, or HyFoSy when foam contrast is used) is widely accepted as a first-line method to assess tubal patency.
Timing & Eligibility: When to Book and When to Wait
Best timing is soon after menstrual bleeding ends but before ovulation (often cycle days 6–10), because the uterine lining is thin and the risk of disturbing an early pregnancy is minimized.
SSG is not performed if pregnancy is possible or when there is an untreated pelvic infection; your clinician will screen for these before scheduling. If you have active pelvic pain or heavy bleeding, the test may be deferred until symptoms settle.
SSG Procedure
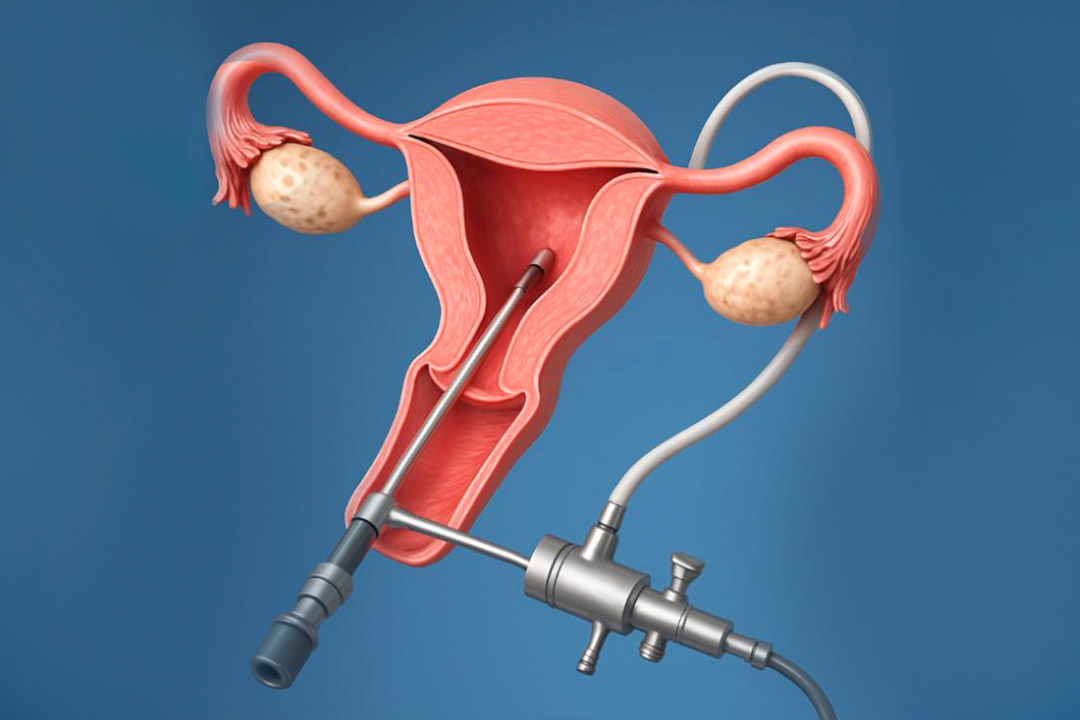
A sonosalpingography (SSG) is an ultrasound-based procedure to check for blockages in the fallopian tubes and assess uterine conditions by injecting a sterile saline solution into the uterus and visualizing its flow.
The process involves inserting a thin catheter into the uterus to introduce the saline, while an ultrasound transducer is used to obtain images of the reproductive organs.
Performed by a radiologist or gynecologist, the procedure is generally safe, non-invasive, takes about 10–30 minutes, and helps in diagnosing infertility and other reproductive issues.
Before the Procedure
The test is typically performed 7-10 days after the start of your menstrual cycle. Preparation: It's advisable to have a full bladder for the procedure. You can discuss options for pain relief, such as oral painkillers or anesthesia, with your doctor.
During the Procedure
- Speculum Insertion: A doctor will perform a gynecological examination with a speculum to visualize the cervix.
- Catheter Placement: A thin catheter is inserted into the uterus.
- Saline Infusion: A sterile saline solution is slowly instilled through the catheter into the uterus to provide clear images.
- Ultrasound Visualization: An ultrasound transducer is used to examine the uterus and fallopian tubes, observing the saline's path to check for any blockages or abnormalities.
Is SSG accurate?
Evidence summaries and guidelines conclude that ultrasound-based tubal testing (HyCoSy/HyFoSy) and X-ray hysterosalpingography (HSG) offer comparable diagnostic capacity for checking whether tubes are open.
Meta-analyses focused on modern ultrasound techniques (including 3D/4D HyCoSy and foam contrast) reinforce high diagnostic performance for detecting tubal occlusion when compared against laparoscopy, the operative “gold standard.”
SSG vs HSG: What You Need to Know
The primary difference is that HSG (Hysterosalpingography) uses X-rays and a contrast dye to visualize the uterus and fallopian tubes, while SSG (Sonosalpingography) uses ultrasound and a sterile saline solution or foam to achieve the same assessment without radiation.
SSG is considered a less invasive, non-radiation alternative to HSG for evaluating the uterine cavity and assessing fallopian tube patency.
Hysterosalpingography (HSG)
An X-ray examination is performed after a contrast dye is injected into the uterus. Purpose: To view the shape of the uterine cavity and check if the fallopian tubes are open. Key Feature: Uses X-rays, which involves a small dose of radiation.
Sonosalpingography (SSG)
An ultrasound-based procedure where a sterile saline solution or foam is injected into the uterus to visualize the reproductive organs. Similar to HSG, it evaluates the uterine cavity and checks for fallopian tube patency.
Key Features- No radiation is a significant advantage, especially for patients who may need multiple scans.
- Often considered more comfortable than HSG.
- Can be a first-line investigation for infertility.
What to Expect and the Rare Events to Know About SSG
SSG/HyFoSy is generally well-tolerated, with the most common effects being transient cramping and light spotting. Safety reviews of the commonly used gel/foam ultrasound contrast report no unexpected serious adverse effects when used as directed.
As with any uterine procedure, rare issues include infection or a brief vasovagal episode (feeling faint). Case reports of unusual reactions exist but are uncommon. If fever, increasing pain, or foul discharge occur after the test, seek medical advice.
A practical advantage of SSG over HSG is no radiation exposure and the ability to evaluate the uterus and ovaries in the same sitting. HSG remains useful especially in some settings but does involve X-ray imaging and iodinated contrast, which is relevant for those with iodine allergy.
Laparoscopy with dye remains the surgical reference test and is reserved for specific indications or when a therapeutic procedure is already planned.
Results & Next Steps After SSG
Reports usually state “both tubes open,” “one tube open,” or “both tubes blocked,” and often comment on the uterine cavity (polyps, fibroids, septum) and ovaries.
If one tube is open, natural conception is still possible; if both appear blocked, your clinician may discuss options that bypass the tubes (for example, IVF) or, in selected cases, further evaluation to confirm and potentially treat the blockage.
Remember that SSG (like HSG) is a high-quality screening test; laparoscopy with dye is the operative reference if surgery is already on the table or endometriosis is strongly suspected.
Costs of Sonosalpingography in India
For SSG/HyCoSy in India, a reasonable ballpark is about ₹3,000–₹7,000, varying with the city, clinic setup, and whether foam contrast or advanced 3D/4D imaging is used.
HSG typically ranges from ₹2,000–₹7,000 in many centres; published lists sometimes show higher figures depending on package components (e.g., anaesthesia, consumables). Always confirm what’s included (scan, disposables, any medications, and the consult to explain results).
Advantages of SSG
Sonosalpingography provides many benefits, such as:
- Radiation-free and clinic-based. Because SSG uses ultrasound, there’s no ionizing radiation. It’s usually done in an outpatient room and takes minutes.
- Two-for-one assessment. The same scan reviews the uterine cavity and ovaries while checking tubal patency, which streamlines early fertility work-ups.
- Comparable accuracy to HSG. Evidence-based guidelines consider HyCoSy/HyFoSy and HSG comparable for confirming tubal patency, allowing choice based on comfort and availability.
- Generally well-tolerated. Cramping is usually brief; serious adverse events are uncommon when the test is done with standard precautions.
SSG, HSG, Laparoscopy: Choosing the Right Test for You
All three have a place, and the “best” option depends on your history and what decisions the result will drive. If radiation avoidance, same-day ultrasound of the pelvis, and clinic convenience matter, SSG is attractive.
If prior imaging is limited and your clinician wants X-ray views of the uterine cavity and tubes, HSG is reasonable. If there’s a strong suspicion of severe endometriosis, adhesions, or a need for concurrent treatment, laparoscopy with dye offers both diagnosis and therapy in the same session.
Shared decision-making is key, guided by your symptoms, prior surgeries or infections, and how the result will influence treatment.
Frequently Asked Questions
Is SSG painful?
Most people feel mild, short-lived cramps—usually seconds to a minute during infusion—then it subsides. Light spotting can occur for a day. Severe pain or fever is not expected; report it if it happens.
Which day of my cycle should I book SSG?
Aim for after bleeding stops and before ovulation (often days 6–10). This timing improves visibility and avoids testing during an early pregnancy.
Can SSG improve my chances of getting pregnant?
SSG’s main role is diagnostic; it tells you whether tubes are open. Some studies of X-ray HSG (especially with oil-based contrast) have reported higher short-term pregnancy rates, but this “tubal flushing” effect is not the primary goal of SSG and remains an area of ongoing research. Your clinician can advise on whether treatment should proceed directly after testing.
Is SSG safe if I have allergies?
Ultrasound contrast foams used in HyFoSy are non-iodinated and have a good safety profile. Rare reactions or vasovagal episodes can occur with any intrauterine procedure; inform your clinician about all allergies and prior reactions.
What if one tube seems blocked?
Conception can still occur if the other tube is open, especially if ovulation alternates. Depending on age, time trying, and other factors, your clinician may suggest trying naturally or proceeding with treatments that bypass or address tubal issues.
Should I think about IVF right away if I am 30?
Not necessarily. If SSG shows both tubes are open and other factors look reassuring, many couples try timed intercourse or simpler treatments first; IVF is typically considered when there are blocked tubes, low sperm parameters, age-related concerns, or when quicker time-to-pregnancy is important. Your individual plan should follow your test results and overall evaluation. (Your clinician will tailor this based on your medical history.)
Do I need antibiotics for SSG?
Routine preventive antibiotics are not universally required, but may be considered if infection risk is higher based on your history or local practice. Follow your clinician’s advice.
Conclusion
Sonosalpingography sits at a practical sweet spot in fertility assessment: it provides a same-day, radiation-free view of the uterus and fallopian tubes with accuracy comparable to long-standing X-ray testing, and without the recovery time of surgery.
Performed in the early part of the cycle, it can clarify whether the tubal pathway is open, reveal uterine findings that may matter for implantation, and help your care team map the shortest, most sensible route to treatment whether that’s expectant management, simpler interventions, or assisted reproduction.
If you’re starting a fertility work-up, asking about SSG is a straightforward way to begin with clear, actionable information.
About Us
AKsigen IVF is a premier center for advanced fertility treatments, with renowned fertility experts on our team. Specializing in IVF, ICSI, egg freezing, and other cutting-edge reproductive technologies, AKsigen IVF is committed to helping couples achieve their dream of parenthood. With personalized care and a patient-first approach, AKsigen IVF provides comprehensive fertility solutions under one roof.